Gum disease treatment
We are UK-qualified clinicians offering professional solutions for minor or advanced gum disease in a state-of-the-art facility designed for your comfort.
We are UK-qualified clinicians offering professional solutions for minor or advanced gum disease in a state-of-the-art facility designed for your comfort.
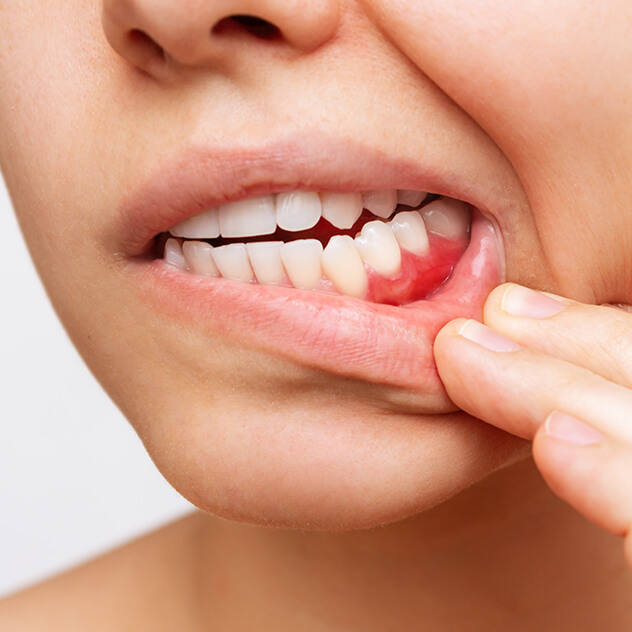
Gum disease, or periodontal disease, destroys the ligaments and bones that hold your teeth in the jaw. It can start as early as your teenage years and is something you may not know you have unless your dentist carefully examines you.
Some common symptoms of gum disease include bleeding gums, gum recession, the development of a space between your teeth and gums, loose teeth, and regular swelling.
Periodontitis cannot be cured but can be held at bay and prevented from advancing further. Once gum disease has presented itself, we recommend that patients establish careful and regular oral hygiene routines.
Specialist treatments for advanced gum disease may include deep cleanings, periodontal check-ups, gum surgery, and bone grafting.
The clinicians and staff at Royston Dental Care are committed to using the latest advancements in dentistry in order to bring you the best preventative care for gum disease.

You may require a periodontal assessment if you have sensitivity, bleeding, or swelling in your gums. Our experienced clinicians will conduct a thorough consultation and offer a customised treatment plan based on your needs.
Book now